Metal Additive Manufacturing for digital dentistry: An introduction for dental professionals
Thanks to a new generation of compact metal Additive Manufacturing machines optimised for dental laboratories, combined with software improvements and optimised workflows, AM technology is now being more widely implemented in medium- to large-sized dental laboratories. In this article, Stijn Hanssen, Director, Dental Applications & Business Development, 3D Systems, reports on the application of metal AM technology for digital dentistry, reducing labour costs, maximising productivity and providing faster outcomes for patients. [First published in Metal AM Vol. 9 No. 1, Spring 2023 | 10 minute read | View on Issuu | Download PDF]

Not long after Chuck Hull filed his first patents for Additive Manufacturing in 1984, the first dental applications were explored, including dental prosthetics and surgical procedures. It was recognised early on that AM brings key advantages for these patient-specific devices which have complex, organic shapes and need to be manufactured as quickly and efficiently as possible.
These first applications were produced using Hull’s polymer Stereolithography (SLA) technology for dental models. This technology – combined with digital processes, software, and materials – enabled new procedures to be addressed with AM whilst accelerating the process. For example, manually creating multiple gypsum models for a single patient with a slight movement of one tooth would not only be very labour intensive, but also potentially inaccurate and unpredictable. Digitally planning these steps, exporting each model to an STL file, and additively manufacturing them reduced the risk of error and was proven to deliver high-quality, accurate devices.
With the development of new dental AM materials that could be certified for biocompatibility, it was also possible to create additively manufactured surgical guides, which opened up the possibility to address a broader range of dental device applications. With the introduction of desktop SLA and, later, digital light processing systems (an early form of Vat Photopolymerisation (VPP) technology) at a fraction of the cost of the first AM machines, the adoption of Additive Manufacturing technology across dental laboratories and dental manufacturing centres rapidly accelerated.
Metal Additive Manufacturing arrives on the scene

With the increasing price of gold and precious metals in the early 2000s, dental technicians began searching for new and more affordable materials for the fabrication of dental crowns. Using the investment casting techniques available at dental laboratories, cobalt chrome (CoCr) – a non-precious metal veneered with ceramics – soon became the standard. When milling machines were introduced, ceramic materials such as zirconia and medical-grade titanium also became a possibility.
Metal Additive Manufacturing was first introduced to the dental industry around ten years ago. Dental metal AM currently uses two materials, CoCr and titanium. CoCr is mainly used for crowns and bridges (which are finished with a tooth-coloured ceramic), as well as for partial dental frameworks or removable partial dentures (RPDs). Titanium is primarily used for implant-supported dentures; titanium structures act as the strong foundation for a denture connected to dental implants.
Just as in polymer AM for dental applications, the key requirements for metal AM in dentistry are reliability, high dimensional accuracy, excellent mechanical properties, and cost effectiveness. Dental restorations, especially those that are manufactured from a digital design file, need to be produced with a high degree of accuracy to ensure a positive patient experience.

When these devices are manufactured using conventional processes, the patient often needs to make multiple visits to the dental office for fittings. In many cases, the final ‘fitting session’ occurs when the prosthetic device is delivered to the patient. Additionally, these devices are used by patients for an extended period and thus must be manufactured from materials that deliver suitable mechanical properties for the intended use.
While metal AM is suitable for some dental device applications, the technology on its own does not always deliver the necessary accuracy and surface finish, and dental products will require additional finishing using traditional technologies. For example, an implant-supported structure requires micron-level accuracy to minimise the likelihood of bacterial infiltration and full arch tension on the jawbone.
This accuracy and surface finish can only be obtained by machining these surfaces in a 5-axis milling machine following the initial metal Additive Manufacturing build process. Likewise, RPDs with a visible metallic palate and clasps require high gloss polishing to minimise plaque accumulation. This can be done manually, but industrial processes such as chemical polishing and dry electro-polishing are also available.
Metal AM process for dental components
In the past decade, dental offices have implemented digital intra-oral scanners and dental laboratories have digitised their gypsum models using desktop scanners. Once a digital representation of the patient’s teeth and/or gums are available, dental CAD software is used to produce a 3D design of the dental restoration. This can be anything from a crown or veneer, to a full denture or orthodontic device. The CAD software usually exports the design as an STL file for manufacturing.
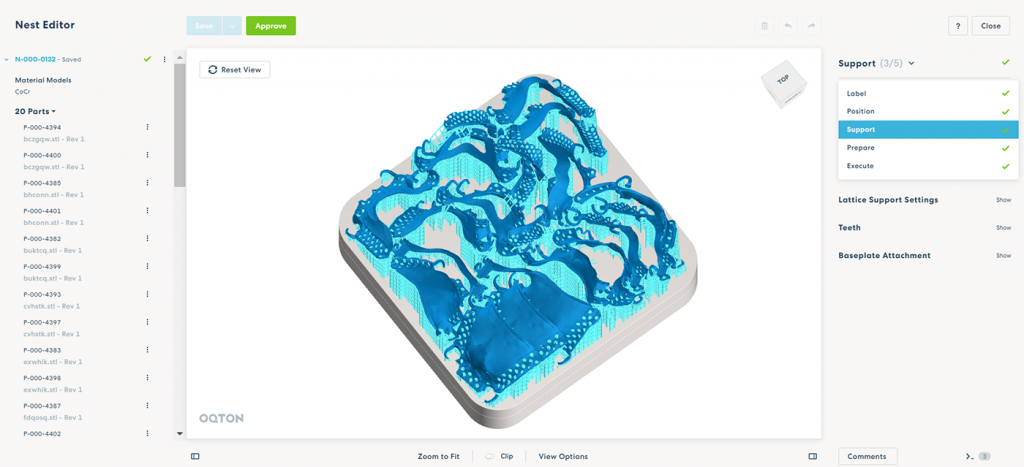
If metal AM is the selected production technology, this STL file is loaded into file preparation software. This software enables the operator to nest different parts into the virtual build volume, move the parts to the optimal orientation, add support structures for the build process, and calculate the build slices for the chosen machine. In recent years, this process has become highly automated and with the recent introduction of artificial intelligence (AI) and machine learning algorithms, it is anticipated that this will soon be an autonomous process.
The AM machine receives the material powder with grain sizes optimised for the machine and application. At 3D Systems, a very small grain size is used on DMP Flex 200 machines for CoCr to obtain the best surface finish and mechanical properties. Once the machine is started, it will first create an inert environment in the build chamber using nitrogen or argon — necessary for AM devices processing titanium. The DMP Flex 200 uses a 500 W laser to selectively melt the cross-sections from the slice file layer by layer to form the part. Virtually created support structures are built with the part to affix it to the build plate, support the overhanging areas, and distribute locally generated heat.
Once the build process is finished, the complete build platform needs to be removed from the machine. The DMP Flex 200 has an airlock system and glove ports to enable this process while minimising the amount of oxygen penetration. This helps to keep downtime between jobs as low as possible. A closed-loop vacuum system extracts used powder for sieving and recycling and can optionally be attached, as well, to further minimise operator time and powder contact.
The build platform with the AM parts attached is now depowdered before being placed in an industrial furnace for an important stress relief process. Depending on the material, this can take up to two hours. For CoCr partials produced on the DMP Flex 200, only thirty minutes at 800°C is required, after which the plate is air cooled to room temperature. After this, the parts can be removed from the platform using pliers or a cutting disc.

Current developments and outlook for dental metal Additive Manufacturing
Until recently, metal AM technology was used mainly by large-scale industrial manufacturing centres available to dental laboratories. Initially, the technology was expensive and required an industrial environment and skilled operators, rendering it inaccessible for most dental laboratories which may have otherwise been interested in incorporating AM.
With recent developments towards machines optimised for dental laboratories (e.g., the DMP Flex 200), software improvements, and optimised workflows, the technology is now available and being implemented in medium- to large-sized dental laboratories. There has been significant adoption of the technology for manufacturing RPDs, to reduce labour and maximise productivity. Additionally, dental implant-supported structures can be post-processed on dental 5-axis milling machines, and this process is offered in cooperation with many different dental CAM software providers.
While metal AM is still in its infancy for digital dentistry compared to resin or polymer AM, recent developments have begun to close the gap. With improvements in hardware, accessories, and software, metal AM machines can now be operated easily inside a dental laboratory and are enabling the efficient production of small, dense, complex dental prostheses with excellent surface quality. In addition to helping laboratories lower their costs, this is also helping dentists deliver a better experience for their patients.

Author
Stijn Hanssen
Director, Dental Applications & Business Development, 3D Systems
www.3dsystems.com







