Bespoke AM knee implants may offer relief to arthritis sufferers
July 16, 2021
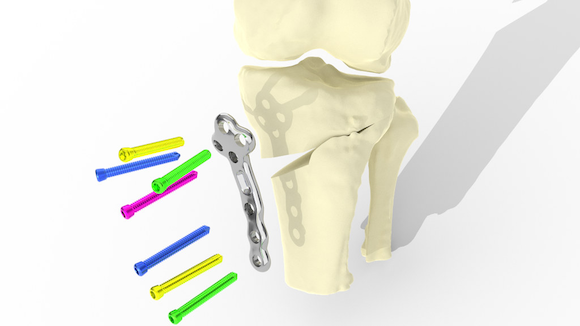
Engineers at the UK’s University of Bath Centre for Therapeutic Innovation (CTI), partnering with 3D Metal Printing Ltd, also in Bath, UK, have developed additively manufactured bespoke titanium alloy plates for the treatment of osteoarthritis in the knee. The TOKA (Tailored Osteotomy for Knee Alignment) is used to preserve the existing joint and can be used at an earlier stage of arthritis, before a knee replacement is needed.
The treatment is said to improve the operative procedure and fit of high-tibial osteotomy (HTO) plates used to realign a patient’s knee, making them more stable, comfortable and better able to bear weight than generic plates. The new technique also simplifies HTO surgery, making operations quicker and safer.
The HTO plates have already been safety tested virtually, in a computer-based trial using the CT scan data of twenty-eight patients. The in-silico trial is reputedly the first in the world to demonstrate the safety of an orthopaedic device, model the stresses that would be exerted on the bespoke plates and show that they would be comparable in safety to the standard treatment.
“Knee osteoarthritis is a major health, social and economic issue and does not receive as much attention as it should,” stated Professor Richie Gill, the Centre for Therapeutic Innovation. “A quarter of women over forty-five have it, and about 15% of men, so it’s a significant burden that many live with.”
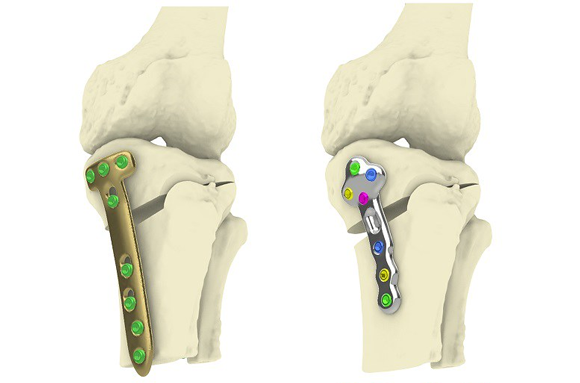
Gill continued, “Knee replacement is only useful for end-stage osteoarthritis, so you can be in pain and have to live with a disability for a long time, potentially decades, before it’s possible. We hope that the new TOKA process we’ve developed will change that.”
Knee osteoarthritis patients undergoing TOKA will undergo a 3D CT scan of their knee, before a personalised AM surgical guide and plate, both shaped to their tibia (shin) bone, is created. The surgical guide simplifies the surgery, and is designed to improve surgical accuracy.
The process is also the first reported implementation of additively manufactured screw threads into the HTO plates, meaning they can be optimally positioned to help secure them against the bone.
High tibial osteotomy surgery realigns the knee joint by making a cut to the shin bone and opening a small gap, which needs to be stabilised with a metal plate. This realignment moves the loading to a less ‘worn’ part of the knee. Patient outcomes depend on how accurately the cut is made and the gap opened. This is where the TOKA method comes in.
“3D printing the custom knee implant and doing the scanning before operating means surgeons will know exactly what they’ll see before operating and where the implant will go,” Gill added. “In addition to a surgeon being able to precisely plan an operation, a surgical guide (or jig) and a plate implant, each personalised to the patient, can be 3D printed automatically based on the scanning data.
The pre-planning element greatly simplifies surgery and could cut the time on the operating table from two hours to around thirty minutes.
In-person trials will begin once clinical centres are reopened for elective surgeries, anticipated to take place later this year. Hospitals in England (Bath, Bristol, and Exeter) and Cardiff, Wales will take part in a randomised control trial to compare patient outcomes with an existing generic HTO procedure.
Tests of the TOKA technique have already begun in Italy, where, thus far, twenty-five patients have received personalised HTO plates as part of a trial at the Rizzoli Institute in Bologna.
The work to date and UK trial is supported and funded by the British arthritis charity Versus Arthritis. The in-silico trial has been published in Communications Medicine.
















